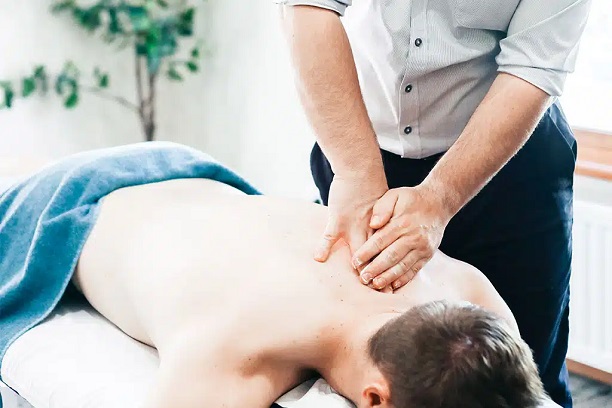
Frozen Shoulder Case Study Mary (not her real name) came to our clinic for treatment for her frozen shoulder. The pain was from the top of her shoulder to her upper arm, and was even more intense when she placed her hand behind her back. (She also felt stiff and sore in her left upper […]